Waking Up … Or Not
Well, as you learned from my last post, I finally decided to have the operation I’d been putting off for years. In the modern medical age it is quite easy to engage in such avoidance; drugs designed to alleviate the most problematic enlarged-prostate symptoms have enabled men to delay surgical intervention for a long time. In my case, I was on Flomax (I’m sure you’ve seen the ads on TV) for about a decade. The ultimate reason for my decision? — the number of trips to the bathroom per unit time was getting pretty damn ridiculous. And, really, I just didn’t feel well anymore.
I’m an academic; I work on a campus. So, given that this was an elective procedure, for a non-life-threatening condition, and in trying to be a most-responsible employee, I thought I should do the operation at the end of Fall semester. Things can be sort of frantic at the end of an academic term, but after that things slow way down and campus is totally closed between Christmas and New Year’s. So, in the middle of November, I scheduled this to happen during the first week of December.
Of course, being the perpetual worrier I am, as I entered the last few days prior to the big event, I became more and more anxious. I had never had a surgery before. And, wouldn’t you know? — I watch all the doctor shows on TV, always have (from Ben Casey and Dr. Kildare, to St. Elsewhere, ER, Chicago Hope, Grey’s Anatomy and House … I’ve always been fascinated). I had good reason to worry, I thought: Murphy’s Law seems to rule. If something can go wrong, it will. Right?

Oh my god, I said to myself. Here I am, 64 years old, and I am having this first-time experience … that could all go terribly, terribly wrong. What would happen if I went under anesthesia and the knife … and then stayed under? You know, like forever! What then?
I have neither a will nor an advanced healthcare directive. Further, there’s the fact that no one is present in my life to provide advocacy for me while I’m in the hospital, no one to make decisions if I don’t wake up, no one who knows what to do in case I die. Shit! Have I really lived this long? Do I really have no one? What the heck do I do NOW?
Well, in the absence of any paperwork, or even having ever talked out any of these issues with anybody, I thought maybe the most responsible thing to do was to let someone in on this particular bout of existential angst.
As it turned out, Katrina and I had been having a brief email exchange about my situation, and in one of her notes, she had asked me about the length of my hospital stay and the anesthesia for my procedure. So I wrote her back telling her what I knew about the spinal anesthesia that would be administered, and then I said…
Speaking of anesthesia … would you consider doing me a favor?
I don’t have a will or an advanced health care directive. If for some reason I don’t wake up from this, could you use this email as evidence of my last wishes? (OK, yes, morbid, I know…)
My last wishes, as of this afternoon, as I write this from a Starbucks in Mill Valley, would be to be cremated with the ashes spread on the top of Mt. Pisgah. If that’s legal up there, that is. So just in case: would you consider communicating this message to my blood relatives — and see if you could make that happen for me?
I will rest easier tonight having said this to someone. If that's too over-the-top a request, just say so, please.
-jim
Thankfully, amazingly, she agreed.
So, yes, thanks again, Katrina. I went into all of this with some peace of mind, imaging myself, in the worst-case scenario, spending eternity on one of my favorite hiking trails in Oregon
Soundtrack Suggestion
All that I know is I’m breathing
All I can do is keep breathing
All we can do is keep breathing
(“Keep Breathing” — Ingrid Michaelson)
[The story continues here.]
A Twist in the Path
I have written before about my old-geezer struggles with benign prostatic hyperplasia (BPH, i.e., “enlarged prostate”), PSA tests, biopsies — and intense discussions with my physicians about interpreting the numbers. August 1999 was the month when a routine blood test yielded a distinctly- elevated PSA, resulting in a referral to a urologist. As it turned out, that appointment was merely the first of many over the intervening years, resulting, so far, in 29 blood tests for PSA, two prostate biopsies, a decade of taking Flomax, and a November 2009 emergency room visit for urinary retention that resulted in catheterization for six days. (Now, that was a memorable Thanksgiving!)
Over 15 years of testing, my PSA numbers have risen steadily (sometimes dramatically), my prostate gland has continued to grow, and my symptoms have become progressively worse. In the course of all those doctor visits, one fact became increasingly evident: should I be so fortunate to keep on living, I would eventually need surgical intervention for my condition.
And, so, that time finally came. During the summer and fall of last year, living with this condition became more and more problematic, and even a double-dose of my medication didn’t provide adequate relief. Reluctantly, very reluctantly, I came to acknowledge that the procedure known as a “TURP” (transurethral resection of the prostate) was imminent.
On December 6, 2011, almost six weeks ago now, I entered Marin General Hospital to have the operation. So, dear reader, be on guard. I’ll be writing more about this journey in coming posts.
[The story continues here.]
Injury, Recovery, Fitness, Health & Change
The Fourth of July this year promised to be a good-weather day for the entire Bay Area, so I took advantage of this prediction and hopped on the 11:40 ferry into the city to spend a few hours doing my walkabout-photography thing. It was a verynice day to do this, as it turned out, so I was feeling pretty pleased with myself (for both the photos and the exercise) as I boarded the 4:30 back to Larkspur. However, despite the incredible, sunny, 70-degree downtown weather, the water in the bay was very choppy, and it was offering up a lot of sea spray as I sat in the back of the boat during the first few minutes of the trip. I decided I didn’t want to endure this for the entire ride and got up to change seats. Just as I stood, the boat took a particularly big jump in the water, and I was tossed onto my backside: my right shoulder hitting one of the solid plastic benches that are permanently affixed to the deck.
As I clumsily pulled myself up, I was in agony. I thought that I’d probably pulled a muscle (or something); I could barely move my arm. I sat there in over-the-top pain for the remainder of the trip, not knowing much except that I’d be making a stop at the emergency room right away. At the ferry landing, I filed an incident report with the ship’s captain, then drove myself, one-armed, to the hospital. Upon examination, and x-ray, the ER staff determined that I had broken my scapula (shoulder blade). Yikes!
I drove home with my arm immobilized in a sling. I endured some pretty incredible, constant pain for the first couple weeks or so. I hibernated for awhile, and stayed away from work, but eventually I started moving again. Within ten days of the incident, I had seen an orthopedist, had a CT and MRI to gather more information (and determined that my shoulder didn’t need surgery), and had kept my first appointment with a physical therapist.
It took about thirteen weeks, a quarter of a year, to get mostly back to “normal.” To facilitate the healing process, I was a model physical-therapy patient, doing my routines at least 2 or 3 times every day. My recovery was “uneventful”, as the orthopedist said, and I feel fine now.
Well, mostly.
The side effect that I didn’t anticipate seems to have been due to my greatly reduced level of physical activity during the recovery period. (At least this is my current working hypothesis.) I have been feeling more and more anxious for several weeks now, including dealing with some pain in my chest (a long-standing anxiety symptom for me). I think the longer I was inactive due to my injury, the less able I was to cope with my myriad, underlying anxiety issues. Of course, the worry haunted me for a quite awhile that this pain wasn’t merely anxiety, but indicative of a heart problem. Hence, I went to see a cardiologist and took a stress EKG test (the one involving a treadmill), along with a stress heart echo (sonogram). According to these procedures, my cardiac function is fine. Whew!
I just joined a local fitness center, and I have my first appointment with a personal trainer this week. I need to get more active, and it seems this would be good way, what with winter coming on and all. (My walking routine typically suffers in bad weather.) Exercise has always been the best way for me to cope with my anxiety and depression woes.
It really is time for a change. Wish me luck.
Soundtrack Suggestion
If you knew that you would be alone,
Knowing right, being wrong,
Would you change?
Would you change?
If you knew that you would find a truth
That brings up pain that can't be soothed
Would you change?
Would you change?
(“Change” - Tracy Chapman)
Social Media & Whatever Happened to the Class of '65
It was a little over two years ago when I first signed up for Facebook and then wrote about my initial experiences and impressions here. At that time, I admitted I had little idea what was I was doing or what it meant to be so affiliated. However, I also reported that, quite rapidly, as a result of Facebook and Twitter, I felt “less alone” in the world.
Time has marched on, and I believe I have a much better handle on the whole social-media scene now than I did then. Over the last couple years, I’ve tweeted and Facebooked (yes, I used that as a verb) much more than anything else I’ve done online, including posting essays here. My level of online activity really hasn’t diminished at all … it just changed direction. The biggest reason, I suppose, is that Facebook and Twitter are much more interactive: there is simply more two-way communication with other people than there ever was with this blog. A lot of the time, this site has been like a very long (and sometimes boring) lecture; Twitter and Facebook have the capacity to be more conversation-like.
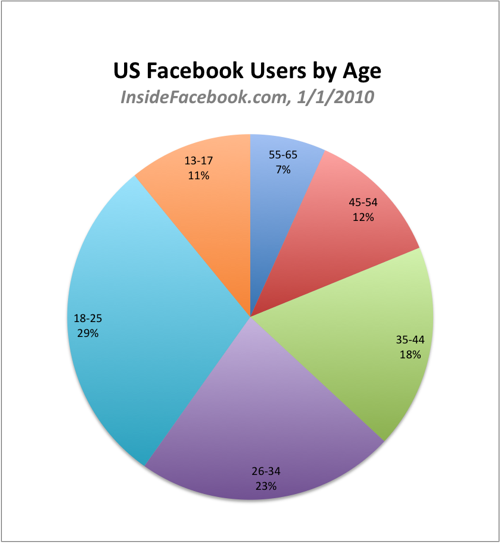
Not everyone is with me here, though … as I am repeatedly reminded. There are tons of people my age who remain as uninterested in online social networking as I once was, and totally stay away from such activity. In fact, I may be the oldest person among my (as of today) 657 followers on Twitter and my 107 friends on Facebook. Earlier this year, I learned that just 7% of all Facebook users are in the 55-65 age bracket (see graph).
So, it would appear that my level of online activity just might put me in the top few percent, or even fraction of one percent, of my contemporaries in terms of social-media savvy.
Apparently, I’m not alone in recognizing my relative uniqueness.
Last weekend was the 45-year reunion of my high school class (in Rice Lake, Wisconsin). I did not attend the gathering because of its rather inconvenient timing (this was the first time we’ve ever held a reunion other than in the summer months). However, I still happened to play a part in the events of last Saturday evening. During the MC’d program after dinner, it was proposed that a class website be set up as we all do the five-year countdown toward our 50th (gasp!) reunion in 2015. One former classmate suggested that the best person for the job would be ME, and, by acclamation, I was elected to make such magic happen.
Hence, being so honored (?), I wrote a few emails, tried to figure out what the heck the expectations were, and just generally spent some time figuring out what we (that is, I) might do.
My decision, supported by those I’ve consulted with, was to construct a group for us all on Facebook, using their just-released (four days ago) “new groups” feature. It is now up and running. (I don’t waste time: give me an assignment, and I do it!) Two days ago I sent out an email to everyone (who submitted an email address to our reunion organizers) announcing the availability of the new group (with some simple instructions about joining Facebook). Right now, we have thirteen members. (I think we have about 200 surviving classmates at this time.)
So, now there’s a small core of us waiting to see how many former classmates will join us in this social network. (I think it would be nice, perhaps amazing, if this experiment actually works!)
Soundtrack Suggestion
When I think back on all the crap I’ve learned in high school
It’s a wonder I can think at all…
(“Kodachrome” – Simon & Garfunkel)
Update on October 11, 2010:
I should acknowledge…
Of course, the title of this entry is somewhat a rip-off of the title of the 1976 book What Really Happened to the Class of ’65? by Michael Medved and David Wallechinsky.
Doctoring in the Western World
Please note:
This long essay (it’s at least four times optimum blog-post length) makes my personal case against the “medical establishment.” I do not take on the insurance companies here, though, but rather the doctors who provide front-line health care for us all.
Although I deal at length with the PSA blood test in the discussion below, I totally omit mention of the controversy currently raging about this procedure.
Caveat lector: this post would likely merit an “R” rating near the end...
I’m one of those old geezers for whom the TV commercials advertising such products as Flomax and Proscar are made: I have an enlarged prostate [benign prostatic hyperplasia (BPH)]. BPH is characterized by a number of urinary symptoms, one of the most obvious being the number of times I have to get up during the night to relieve myself. (For a list of other symptoms, click here.)
As I have monitored my condition over the last 12 years, with the assistance of various urologists in the cities I have lived, I have regularly (at least every six months) undergone the blood test for prostate specific antigen (PSA), the front-line screening protocol for prostate cancer. During this time, as my prostate has grown in size, my PSA has risen slowly, steadily, but not dangerously. I keep track of the results by means of an Excel spreadsheet and graph, and even furnish my doctors with a least-squares plot of these data at every appointment. At one point, back in late 2002, there was an unusual spike in the one of the readings, and I was advised to have a prostate biopsy. This procedure is a very invasive and uncomfortable one, but I went ahead, in early 2003, and did it anyway. After eight full days anxiously waiting, I finally was informed that the result was negative. Since that time I have simply continued to monitor the slow, steady, predictable rise of my PSA level.
Well: except that that all changed recently. In both January and March of this year, my PSA tests have yielded significantly higher readings – data that do not fit neatly within the paradigm of my least-squares analysis. After the January result, my urologist reacted as I did: one test alone means nothing. Let’s wait a bit (a few weeks) and do it over again.
And that’s what we did, though the second test in March indicated a slightly elevated level compared to the January number. It was at this point that he stated that it was time for concern and said, “you know where we go from here.” He meant a biopsy, of course, and I declined, indicating that I wanted to wait for one more blood (PSA) test before undergoing that procedure again.
However, he was very insistent that we do a biopsy, and I was just as opinionated that it was not yet time. I told him that I had one more hypothesis to test out before I would submit to the procedure. Simply put, my theory is: my PSA number is inflated due to a new dietary supplement I had started taking. Last October (over two months prior to the January blood test), I began a product called ArthroZyme, advertised as an anti-inflammatory agent, to see if it would help me out with the chronic muscle pain that has plagued me for the last few years. The active ingredient in this product is a proteolytic enzyme called serratiopeptidase. And, as it turns out, PSA itself is itself a proteolytic enzyme. I believe it is much more than coincidental that immediately after I began taking a proteolytic enzyme supplement I start testing differently for a specific proteolytic enzyme. I believe the two phenomena are connected and that this is the simplest possible, and most likely, explanation. I contend that this hypothesis is one that merits serious consideration, and that I should, therefore, simply stop taking the supplement and re-test.
As it turned out, I was only able to leave the urologist’s office in early April after hearing the strongest language he could muster that I was making a mistake and the he strongly recommended this test. NOW.
Of course, I don’t think I’m being at all unreasonable.
I’m the guy, after all, who was told, by TWO doctors, in no uncertain terms, one night in an emergency room, that he had bladder cancer. But I didn’t, as the cystoscopy (now there’s an invasive procedure), performed a couple of days later in a doctor’s office, conclusively demonstrated.
I’m the one who submitted to a biopsy back in 2003 on the basis of a PSA spike. And I didn’t have cancer, then, either.
I’m the one who has been totally discounted by my primary care physician, to the point of being told that my body aches and pains were “psychiatric” in origin and that the supplements I take (and rely on) couldn’t possibly be doing me any good.
And, I’m the person who was kept waiting for a half hour in a neurologist’s office after having experienced the intake nurse botch the explanation of my test results – only to finally talk to the doctor and learn that the (MRI) result in question was inconsequential.